Know Your Body, Improve Your Health
Taking the time to understand how your body works is one of the smartest steps you can take for your overall well-being. While most health discussions focus on muscles and movement, pelvic health is just as important—especially for men, who often receive limited education in this area.
The male pelvic region plays a key role in urinary control, sexual function, and physical stability. When something feels off—whether it’s discomfort, changes in urination, or sexual health concerns—having a basic understanding of your anatomy can make it easier to identify issues and seek the right care.
Let’s break down the essential external and internal structures that support male pelvic health.
External Organs
These are the visible parts of the male reproductive system, responsible for protection, hormone production, and sexual function.
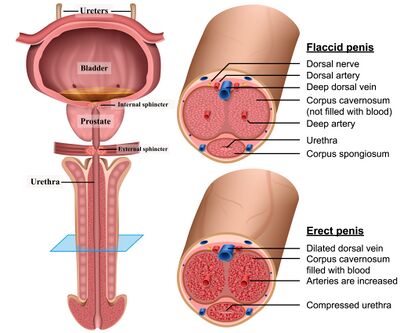
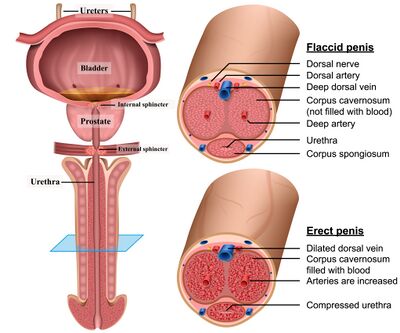
Penis
The penis serves both urinary and reproductive functions. It contains the urethra, which carries urine out of the body.
Structurally, it consists of three columns of erectile tissue:
- Corpora cavernosa (2): Fill with blood to create an erection
- Corpus spongiosum: Surrounds the urethra and keeps it open during ejaculation
At the tip is the glans, a highly sensitive area rich in nerve endings. Proper blood flow, nerve health, and pelvic muscle support all contribute to healthy erectile function.
Testicles (Testes)
The testicles are responsible for producing sperm and testosterone—the primary male hormone.
Testosterone supports:
- Muscle growth
- Bone density
- Energy levels
- Libido
- Sperm production
Inside the testicles are tiny tubes where sperm is formed. It then moves to the epididymis, where it matures and is stored.
Scrotum
The scrotum is the sac of skin that holds and protects the testicles. Its main job is temperature regulation.
Since sperm production requires a slightly cooler environment, the scrotum adjusts automatically:
- Pulls the testicles closer in cold conditions
- Relaxes and lowers them in warmer temperatures
It also contains muscles and connective tissue that help protect the area and support surrounding pelvic structures.
Internal Organs
These structures work behind the scenes to support reproduction and urinary function.
Urethra
The urethra is a tube that carries urine from the bladder out of the body. In men, it also transports semen during ejaculation.
Two muscles control its function:
- Internal sphincter: Manages involuntary urine flow
- External sphincter: Allows voluntary control
Proper coordination between the bladder, urethra, and pelvic floor is essential for normal urinary function.
Prostate
The prostate is a small gland located below the bladder and around the urethra. It produces fluid that nourishes and protects sperm.
As men age, the prostate may enlarge—a condition known as benign prostatic hyperplasia (BPH). This can lead to:
- Frequent urination
- Difficulty starting urination
- Weak urine flow
- Feeling of incomplete bladder emptying
Routine checkups are important for maintaining prostate health.
Vas Deferens & Ejaculatory Ducts
These tubes transport sperm through the reproductive system.
- The vas deferens carries sperm from the epididymis
- The ejaculatory ducts combine sperm with fluids from the prostate and seminal vesicles
This mixture forms semen, which exits through the urethra during ejaculation.
Why Pelvic Health Matters
Pelvic health isn’t just a women’s issue—it’s essential for men too. The pelvic floor muscles support key organs and help regulate:
- Urination
- Bowel movements
- Sexual function
When these muscles aren’t functioning properly, symptoms may include:
- Pelvic or groin pain
- Urinary urgency or leakage
- Erectile dysfunction
- Pain while sitting
- Discomfort during or after ejaculation
In many cases, targeted therapies—like pelvic floor physical therapy—can help restore balance, reduce tension, and improve function.
The Bottom Line
Understanding your pelvic anatomy isn’t just about knowledge—it’s about taking control of your health. Recognizing early signs of imbalance can help you act sooner, avoid complications, and have more confident conversations with healthcare professionals.
If you’re experiencing discomfort or changes in function, don’t ignore it. Getting the right guidance can make a significant difference in your long-term health and quality of life.