Abstract
Objectives
The aim of this study was to identify risk factors of in-hospital mortality among diabetic patients infected with COVID-19.
Study design
Retrospective cohort study.
Methods
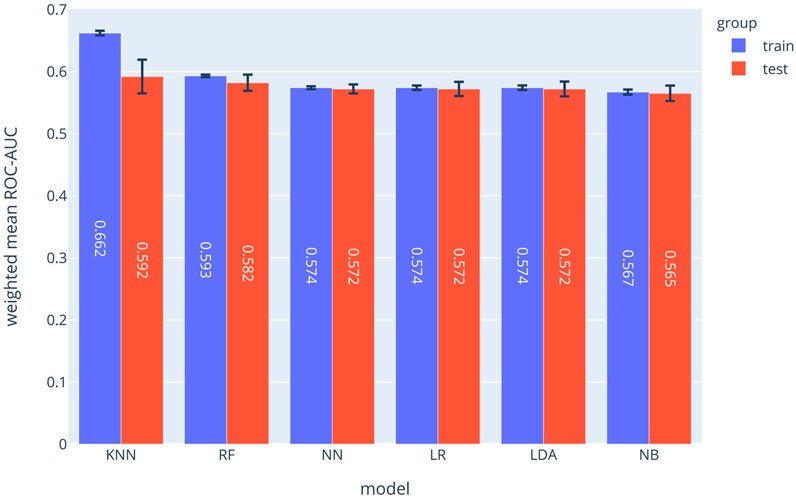
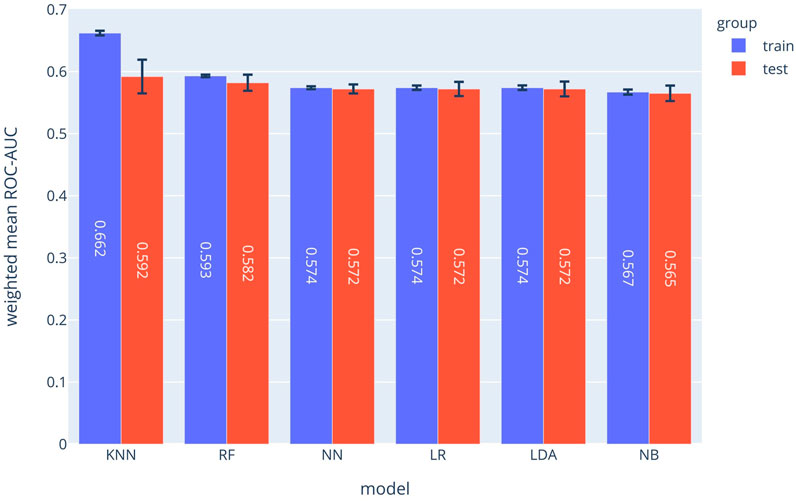
Using logistic regression analysis, the independent association of potential prognostic factors and COVID-19 in-hospital mortality was investigated in three models. Model 1 included demographic data and patient history; model 2 consisted of model 1, plus vital signs and pulse oximetry measurements at hospital admission; and model 3 included model 2, laboratory test results at hospital admission. The odds ratios (ORs) and 95% confidence intervals (95% CIs) were reported for each predictor in the different models. Moreover, to examine the discriminatory powers of the models, a corrected area under the receiver-operating characteristic curve (AUC) was calculated.
Results
Among 560 patients with diabetes (men = 291) who were hospitalised for COVID-19, the mean age of the study population was 61.8 (standard deviation [SD] 13.4) years. During a median length of hospitalisation of 6 days, 165 deaths (men = 93) were recorded. In model 1, age and a history of cognitive impairment were associated with higher mortality; however, taking statins, oral anti-diabetes drugs and beta-blockers were associated with a lower risk of mortality (AUC = 0.76). In model 2, adding the data for respiratory rate (OR 1.07 [95% CI 1.00–1.14]) and oxygen saturation (OR 0.95 [95% CI 0.92–0.98]) slightly increased the AUC to 0.80. In model 3, the data for platelet count (OR 0.99 [95% CI 0.99–1.00]), lactate dehydrogenase (OR 1.002 [1.001–1.003]), potassium (OR 2.02 (95% CI 1.33–3.08]) and fasting plasma glucose (OR 1.04 [1.02–1.07]) significantly improved the discriminatory power of the model to AUC 0.86 (95% CI 0.83–0.90).
Conclusions
Among patients with type 2 diabetes, a combination of past history and pulse oximetry data, with four non-expensive laboratory measures, was significantly associated with in-hospital COVID-19 mortality.
[“source=sciencedirect”]